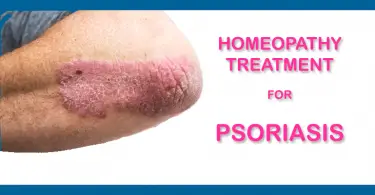
This article deals with the homeopathy treatment of Multiple sclerosis with most commonly indicated homeopathic medicines for Multiple sclerosis.
Multiple sclerosis is a chronic, degenerative, typically progressive autoimmune disease causing damage to the sheaths of neurons in the brain and spinal cord.
In multiple sclerosis, multiple scar forms on the covering of neurons (myelin sheath) that affects the ability of neurons to carry signals between brain and body results in,
- Numbness,
- Impairment of speech
- Muscular coordination,
- Blurred vision
- Severe fatigue etc.
Multiple sclerosis is an inflammatory demyelinating disease on CNS (brain and spinal cord) that is disseminated in time and space. Multiple sclerosis cannot be diagnosed until patient has suffered attacks involving different neuroanatomical site at different times.
An acute multiple sclerosis plaque develops when primed leucocytes cross the blood brain barrier into the brain, and activates macrophages. Inflammation is initiated and myelin is stripped off near nerve axoms. These nerves lose the ability to conduct impulses.
Although many patients lead full and rewarding lives, MS can cause impaired mobility and disability in the more severe cases.
Multiple sclerosis attacks neurons, the cells of the brain and spinal cord that carry information, create thought and perception, and allow the brain to control the body. Surrounding and protecting these neurons is a layer of fat, called myelin, which helps neurons carry electrical signals.
MS causes gradual destruction of myelin (demyelination) in patches throughout the brain and/or spinal cord. Myelin not only protects nerve fibers, but makes their job possible. When myelin or the nerve fiber is destroyed or damaged, the ability of the nerves to conduct electrical impulses to and from the brain is disrupted, and this produces the various symptoms of MS.
The illness takes the form of repeated exacerbation (aggravation leading to an attack). For no known reason, the exacerbation usually stops of its own accord, and period of remission follows when the disease is not active.
The name multiple sclerosis refers to the multiple scars (or scleroses) on the myelin sheaths. MS results from attacks by an individual’s immune system on his or her own nervous system, and it is therefore categorized as an autoimmune disease.
Multiple sclerosis can take several different forms, with new symptoms occurring in discrete attacks or slowly accruing over time. Between attacks symptoms may resolve completely, but permanent neurologic problems often persist.
MS primarily affects adults, with an age of onset typically between 20 and 40 years, and is more common in women than in men.
Homeopathy Treatment for Multiple sclerosis
Aim of homeopathy treatment for Multiple sclerosis includes:
- Treatment of a patient without giving him another new suffering (side effects)
- Patients are treated holistically for all presenting symptoms; do not need separate medicine for each set of symptom.
- To improve patients vitality without suppression.
Homeopathy is one of the most popular holistic systems of medicine. The selection of homeopathic remedy is based upon the theory of individualization and symptoms similarity by using holistic approach.
This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering.
The aim of homeopathic medicines for Multiple sclerosis is not only to treat symptoms of Multiple sclerosis but to address its underlying cause and individual susceptibility.
As far as homeopathic medicine for treatment of multiple sclerosis is concerned, several well-proved homeopathy medicines are available for symptoms of multiple sclerosis treatment that can be selected on the basis of cause, sensations, modalities and extension of complaints.
The homeopathic medicines for multiple sclerosis given below indicate the therapeutic affinity but this is not a complete and definite guide to the treatment of multiple sclerosis.
The symptoms listed against each medicine may not be directly related to this disease because in homeopathy general symptoms and constitutional indications are also taken into account for selecting a homeopathic medicine for multiple sclerosis.
For individualized remedy selection and homeopathic treatment, the patient should consult a qualified homeopathic doctor in person.
Following homeopathic medicines cover symptoms of various types and stages of Multiple Sclerosis:
– Begins in lower limb – con.
– Double vision, with – gels
– Grief from – caust, con, phos, nat-m
– Influenza shots after – gels
– Softening of spinal cord, with – arg-n, atro, aur, crot-h, lah, phos, phys, plb, stry, chel, ox-ac, tarent, thuja, sulph, bar-c, bell, gels, lyc, nux-v, sil, calc.
– Vertigo, with – conium.
Common homeopathy medicines for Multiple sclerosis
- Causticum
- Gelsemium
- Oxalic acid
- Phosphorus
- Natrum muriaticum
- Conium maculatum
- Plumbum metallicum
- Zincum metallicum
- Cuprum metallicum
- Syphilinum
- Cicuta virosa
The detail symptoms of these homeopathic remedies for MS are as follows:
Causticum
- Homeopathy medicine for multiple sclerosis with chronic paralytic affections indicated by tearing, drawing pains and severe weakness.
- Local paralysis, paralysis of vocal cords, tongue, eyelids, face, bladder and extremities.
- Paralysis of single parts ofextremities with dull, tearing pains and loss of sensation.
- Impaired vision with sparks and dark spots before eyes. Ptosis and paralysis of extra ocular muscles.
- Restless legs at night with weak ankles.
- Better by warmth especially heat of bed.
- Paralysis of bladder with involuntary urination on sneezing and coughing.
Gelsemium
- Center its action on nervous system and brain and thus causes varying degrees of motor paralysis.
- General prostration with dizziness, dullness,trembling and drowsiness. Paralysis of various groups of muscles about eyes, throat, larynx, extremities etc.
- Muscular weakness and complete relaxation.
- Lack of muscular co-ordination. Ptosis, eyelids heavy, patient can hardly open them with double vision.
- Vision blurred and smoky. Dim sighted with orbital neuralgia.
- Cramps in muscles with profuse, clear, watery urine and chilliness and tremulousness.
- Partial paralysis of bladder.
Oxalic acid
- Multiple cerebral and posterior spinal sclerosis.
- Lancinating, shooting and jerking pains in various parts.
- Muscular prostration. Numb, weak and tingling sensation. Backache with numbness.
- Paralysis with pains very violent and in small spots worse motion and thinking about them.
- Drawing and lancinating pains shooting down the extremities.
Phosphorus
- Produces softening and atrophy of brain and spinal cord causing marked prostration and trembling, numbness with complete paralysis
- Sensory and motor paralysis from ends of fingers and toes.
- Weakness and trembling from every exertion. Arms and hands become numb. Can scarcely hold anything.
- Great susceptibility to external impressions as light, sound, touch, thunders. Black points seem to float before the eyes.
- Fatigue of eyes and head with hands.
Natrum muriaticum
- Multiple sclerosis with painful contractions of muscle of thigh.
- Ankles weak and turn easily. Coldness of legs with congestion of head, chest and stomach.
- Eyelid heavy. See sparks. Fiery zigzag lines running.
- Emaciated patient with great weakness and emaciation. Psychic causes of diseases and ill effects of grief, fright and anger. Consolation aggravates.
Argentum nitricum
- The neurotic effects in this drug are very marked, many brain and spinal symptoms are present.
- Symptoms of in-coordination, loss of control and want of balance every where.
- Trembling in affected parts with great desire for sweets.
- Spots before eyes. Eye strain from sewing worse in warm room. Blurred vision.
- Trembling with general debility.
Conium
- It is an excellent remedy for old age problems of weakness, languor, local congestions and loss of strength
where difficult gait, trembling and painful stiffness of legs are often found.
- It corresponds to debility, urinary troubles, weakened memory and eye troubles.
- Eyes – dim sighted worse artificial lights. Paralysis of ocular muscles.
- Heavy, weary, paralyzed and trembling unsteady hands. Numbness of toes and fingers.
Plumbum metallicum
- This is a great homeopathy medicine for multiple sclerosis for sclerotic conditions causes paralysis chiefly of extensor, forearm or upper limb from centre to periphery with partial anesthesia or excessive hyperesthesia preceded by pain.
- Localized neuralgic pains with neuritis.
- Eyes – sudden loss of sight after fainting.
- Paralysis of single muscles. Cannot raise arms, can’t lift anything. Extension is difficult. Paralysis from overexertion of extensor muscles in piano players.
Homeopathic medicines are selected on the basis of symptoms, cause, family history and constitution of the person affected. Considering all these factors any of the above (or some other) homeopathic medicine may be indicated and helpful in a case of Multiple Sclerosis.
Types of Multiple sclerosis
It is an autoimmune disease represents itself by variety of symptoms. According to the appearance and progression of symptoms National Multiple Sclerosis Society (NMSS) is divided multiple sclerosis into four forms.
- Relapsing-remitting (RRMS)
- Primary-progressive (PPMS)
- Secondary-progressive (SPMS)
- Progressive-relapsing (PRMS)
– Relapsing-Remitting Multiple Sclerosis
Characteristics: People with this type of MS experience clearly defined flare-ups or relapses. These are episodes of acute worsening of neurologic function. They are followed by partial or complete recovery periods (remissions) free of disease progression.
Frequency: Most common form of MS at time of initial diagnosis. Approximately 85%.
– Primary-Progressive Multiple Sclerosis
Characteristics: People with this type of MS experience a slow but nearly continuous worsening of their disease from the onset, with no distinct relapses or remissions. However, there are variations in rates of progression over time, occasional plateaus, and temporary minor improvements.
Frequency: Relatively rare. Approximately 10%.
– Secondary-Progressive Multiple Sclerosis
Characteristics: People with this type of MS experience an initial period of relapsing-remitting disease, followed by a steadily worsening disease course with or without occasional flare-ups, minor recoveries (remissions), or plateaus.
Frequency: 50% of people with relapsing-remitting MS developed this form of the disease within 10 years of their initial diagnosis, before introduction of the “disease-modifying” drugs. Long-term data are not yet available to demonstrate if this is significantly delayed by treatment.
– Progressive-Relapsing Multiple Sclerosis
Characteristics: People with this type of MS experience a steadily worsening disease from the onset but also have clear acute relapses (attacks or exacerbations), with or without recovery. In contrast to relapsing-remitting MS, the periods between relapses are characterized by continuing disease progression.
Frequency: Relatively rare. Approximately 5%.
Symptoms of Multiple sclerosis
The most common symptoms of Multiple sclerosis MS include:
- Neck flexion induces electric shock like sensation running down the back.
- Pain in one eye, particularly on eye movements
- Dimness of vision, Diplopia
- Numbness
- Sensation of cold water running down the back
- Stiffness of back
- Flexor spasms, cramps
- Ataxia of limbs, unsteady gait
- Fatigue
- Erectile dysfunction
- Constipation
- Slurred speech
- Poor memory
- Epilepsy
- Personality changes
- Absent abdominal reflexes
- Urinary frequency and retention
- Weakness or numbness of face
Individuals with multiple sclerosis may experience a wide variety of symptoms. The initial attacks are often transient, mild (or asymptomatic), and self-limited. They often do not prompt a health care visit and sometimes are only identified in retrospect once the diagnosis has been made based on further attacks.
The most common initial symptoms reported are: changes in sensation in the arms, legs or face (33%), complete or partial vision loss (optic neuritis) (16%), weakness (13%), double vision (7%), unsteadiness when walking (5%), and balance problems (3%). Fifteen percent of individuals have multiple symptoms when they first seek medical attention.[3]
Most people find their initial MS symptoms occur over a period of hours to weeks. For some people the initial MS attack is preceded by infection, trauma or strenuous physical effort.
Other symptoms and physical findings common in MS are flickering eye movements (nystagmus), speech difficulties, tremor, clumsiness of the hands, abnormal muscle spasms, bladder and bowel difficulties, and sexual dysfunction.
Cognitive impairments are also common, such as difficulty performing multiple tasks at once, difficulty following detailed instructions, loss of short term memory, emotional instability, and fatigue.
Emotional symptoms are common and can be the normal response to having a debilitating disease or the result of damage to the nerves that generate and control emotions.
The most common condition, clinical depression, is a product of both causes. Feelings such as anger, anxiety, frustration, and hopelessness are also common, and suicide is a very real threat.
Cause of Multiple sclerosis
MS is an autoimmune disease and there is not a single definitive cause which is responsible for the disease. There are multiple factors like genes, family history, vit-D deficiency, and certain infections which make a person prone to have multiple sclerosis.
Family history- A person with positive family history of multiple sclerosis in parents and sibling are at high risk of having multiple sclerosis.
Vitamin D- Many researchers suggest that vitamin D support and strength immune system and reduce risk of autoimmune disease. People having low vitamin D level are at more risk to develop autoimmune disease.
Environmental factors –Multiple sclerosis is less prevalent in tropical countries, (countries near to equator) which again support the role of vitamin D in multiple sclerosis. People who live closer to the equator are exposed to greater amounts of sunlight year round. As a result, they tend to have higher levels of naturally produced vitamin D
Smoking- There are certain studies that prove a connection between smoking and multiple sclerosis. Smoking increases risk of having multiple sclerosis if a person is genetically predisposed or has positive family history. Fortunately, the evidence also suggests that stopping smoking whether before or after the onset of multiple sclerosis decrease rate of progression of disability.
Infections -Researchers haven’t yet identified any infectious agent that definitely causes MS but there is growing evidence that certain infections could contribute to someone’s risk of developing MS.
People infected with Epistein-barr virus, Human herpes virus 6, Clostridium perfringens type B, Chlamydophila pneumoniae are on higher risk of developing multiple sclerosis than the people never had these infections.
Obesity- Obese people are on higher risk of getting multiple sclerosis if they are genetically predisposed. This might be because obese people are often low in vitamin D. Obesity can also make immune system overactive and cause inflammation in body.
Prognosis of Multiple Sclerosis
For a person with multiple sclerosis the prognosis depends on the sub type of disease , the individual’s sex , race , age and initial symptoms.; and the degree of disability the person experiences.The life expectancy is high due to improved methods of limiting disability like physical therapy , occupational therapy and speech therapy.
Individuals with progressive sub types , particularly primary progressive have a more rapid decline of functions. In the primary progressive subtype , supportive equipment as wheel chair or standing frame is often needed.
The earlier in life MS occurs , the slower disability progresses.Individuals who are older than fifty when diagnosed are more likely to experience a chronic progressive course.
Those diagnosed before age 35 have the best prognosis. Females generally have beter prognosis than males.
Initial MS symptoms of visual loss or sensory problems such as numbness or tingling are markers for a relatively good prognosis but difficult walking and weakness are signs of poor outcome.
Diagnosis of Multiple Sclerosis
Currently there are no clinically established laboratory investigations available that can predict prognosis or response to treatment. However some promising approaches have been proposed. These include measurement of the two antibodies anti-myelin oligodendrocyte glycoprotein and anti-myelin basic protein .
In addition to a complete medical history and physical examination, a neurological examination, your doctor may order blood tests and refer you to a neurologist (a doctor with specialized training in diseases of the nervous system). Your doctor may also order an MRI scan of your brain and/or spinal cord to look for the characteristic patches of MS and may perform a lumbar puncture (“spinal tap”)—sampling of thecerebrospinal fluid (the fluid that surrounds the brain and spinal cord)—to analyze for proteins associated with the disease.
Treatment for Multiple Sclerosis
There is as yet no cure for MS in conventional medicine. Many patients do well with no therapy at all, especially since many medications have serious side effects and some carry significant risks. However, three forms of beta interferon (Avonex, Betaseron, and Rebif) have now been approved by the Food and Drug Administration for treatment of relapsing-remitting MS. Beta interferon has been shown to reduce the number of exacerbations and may slow the progression of physical disability. When attacks do occur, they tend to be shorter and less severe. The FDA also has approved a synthetic form of myelin basic protein, called copolymer I (Copaxone), for the treatment of relapsing-remitting MS. Copolymer I has few side effects, and studies indicate that the agent can reduce the relapse rate by almost one third. An immunosuppressant treatment, Novantrone (mitoxantrone ), is approved by the FDA for the treatment of advanced or chronic MS.
While steroids do not affect the course of MS over time, they can reduce the duration and severity of attacks in some patients. Spasticity, which can occur either as a sustained stiffness caused by increased muscle tone or as spasms that come and go, is usually treated with muscle relaxants and tranquilizers such as baclofen, tizanidine, diazepam, clonazepam, and dantrolene.
Physical therapy and exercise can help preserve remaining function, and patients may find that various aids — such as foot braces, canes, and walkers — can help them remain independent and mobile. Avoiding excessive activity and avoiding heat are probably the most important measures patients can take to counter physiological fatigue. If psychological symptoms of fatigue such as depression or apathy are evident, antidepressant medications may help.
Drug therapies—Medications that target the body’s immune system may decrease the frequency and duration of attacks. These medications can be used on a long-term basis and also to treat specific attacks. Additional medications may be prescribed for other symptoms, such as pain or depression.
Additional therapies—Because MS may affect the patient’s ability to perform self-care and other activities of daily living, treatment may also include referral to specialists for physical and occupational therapy
Many patients do well with no therapy at all, especially since many medications have serious side effects and some carry significant risks. However, three forms of beta interferon (Avonex, Betaseron, and Rebif) have now been approved by the Food and Drug Administration for treatment of relapsing-remitting MS.
Beta interferon has been shown to reduce the number of exacerbations and may slow the progression of physical disability. When attacks do occur, they tend to be shorter and less severe.
The FDA also has approved a synthetic form of myelin basic protein, called copolymer I (Copaxone), for the treatment of relapsing-remitting MS. Copolymer I has few side effects, and studies indicate that the agent can reduce the relapse rate by almost one third. An immunosuppressant treatment, Novantrone (mitoxantrone), is approved by the FDA for the treatment of advanced or chronic MS.
While steroids do not affect the course of MS over time, they can reduce the duration and severity of attacks in some patients. Spasticity, which can occur either as a sustained stiffness caused by increased muscle tone or as spasms that come and go, is usually treated with muscle relaxants and tranquilizers such as baclofen, tizanidine, diazepam, clonazepam, and dantrolene.
Physical therapy and exercise can help preserve remaining function, and patients may find that various aids — such as foot braces, canes, and walkers — can help them remain independent and mobile. Avoiding excessive activity and avoiding heat are probably the most important measures patients can take to counter physiological fatigue.
If psychological symptoms of fatigue such as depression or apathy are evident, antidepressant medications may help. Other drugs that may reduce fatigue in some, but not all, patients include amantadine (Symmetrel), pemoline (Cylert), and the still-experimental drug aminopyridine. Although improvement of optic symptoms usually occurs even without treatment, a short course of treatment with intravenous methylprednisolone (Solu-Medrol) Followed by treatment with oral steroids is sometimes used.
Main conventional drugs used are –
Avonex.
Betaseron.
Betaferon.
Copaxone.
Rebif.
Main side effects of these drugs:
A) Avonex
Anaphylaxis.
Autoimmune disorders.
Cardiomyopathy.
Congestive heart failure.
B) Rebif
Anaphylaxis.
Autoimmune disorders.
Depression and suicide.
Flu like symptoms.
Hepatic injury.
Hepatitis.
Injection site reactions.
Pregnancy.
Psychiatric disorders.
Seizures.
Thyroid malfunctions.
C) Copaxone
Adverse effects.
Anaphylaxis.
Flu like reactions.
Menstruation and abnormal bleeding.
Seizures.
Decreased peripheral blood counts.
D) Betaseron
Renal and urogenital dysfunctions.
Multiple Sclerosis Cases Cured with Homeopathic Medicine
Reversal of Multiple Sclerosis in a Woman of 53 – by Domenic Stanghini
Multiple Sclerosis in a Man of 55 – by Peter Naydenov
CASE OF MULTIPLE SCLEROSIS AND TRIGEMINAL NEURALGIA – by Kate Hudson, Christiane Magee



 where difficult gait, trembling and painful stiffness of legs are often found.
where difficult gait, trembling and painful stiffness of legs are often found.