Blood pressure is the pressure or force of blood exerted upon the walls of the arteries as the heart pumps out blood. Blood pressure is measured as systolic and diastolic. Normal value of blood pressure in adults is 120/80 mm.Hg.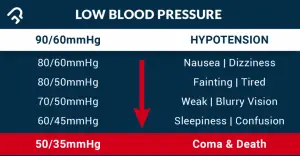
Homeopathic treatment of low blood pressure
Homeopathy is one of the most popular holistic systems of medicine. The selection of remedy is based upon the theory of individualization and symptoms similarity by using holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathy is not only to treat low blood pressure but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to treat low blood pressure that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person.
The most commonly indicated homeopathic medicines in low blood pressure are:
Carbo-veg, Phos, Sepia, Thyroidinum, Baryta-mur, Aconite, Aranea, Cactus, Curare, Gelsemium, Halo, Histamine, Lachesis, Lyco, Naja, Rauwolfia, Reserprine, Visc., Radium, Theridion, Oleander, Laurocrasis, Acid flour, Adrenalin, Ars alb, Aurum mur, Bartya carb, Bryonia, Crataegus China, Conium, Ferrum met, lycopus, Nat mur, Pulsatilla.
There are following remedies which are helpful in the treatment of low blood pressure:
Cactus – low blood pressure, due to cardiac disease; pulse feeble, irregular, quick, without strength; angina pectoris, cold sweat and iron band feeling all the time; endocarditis with mitral insufficiency; temperature subnormal; endocardial murmurs, excessive impulse.
Camphor – low blood pressure, pulse small and weak, sudden sinking of the strength, icy coldness of the whole 
Carbo veg – disintegration and imperfect oxidation is the keynote of this remedy; low blood pressure; persons who have never fully recover from the effects of some previous illness.
Crataegus – it is a heart tonic; prevents sudden fall in blood pressure; extreme dyspnoea and weakness; very feeble and irregular heart action.
Radium brom – lowered blood pressure; great weakness; hypotension due to severe pain in different parts of the 
Kali phos – considered as brain tonic, great nervous exhaustion; low blood pressure due to nervousness; great prostration and weakness.
Natrum mur – heat of sun is unbearable; patients with great craving for salt; great debility and weakness felt in the morning in bed; hypotension may arise from anemia; oversensitive to all impressions; corrects low blood pressure symptoms due to Addison’s disease.
China off – low blood pressure due to loss of vital fluids; from dehydration or diarrhea, vomiting; after sexual excess of loss of semen
Lycopodium – hypotension along with gastric disturbances; great desire for sweets.
Causes of Low Blood Pressure
Conditions that reduce the volume of blood, reduce cardiac output (the amount of blood pumped by the heart), and medications are frequent causes of low blood pressure.
Causes of low blood pressure due to low blood volume
• Dehydration is common among patients with diarrhea who lose large amounts of water in their stool, particularly when drowsiness limits their drinking of fluids or is associated with nausea and vomiting. Dehydration also can occur with prolonged vomiting of any cause because of the loss of water in the vomitus. Other causes of dehydration include exercise, sweating, fever, and heat exhaustion or heat stroke. Individuals with mild dehydration may experience only thirst and dry mouth. Moderate to severe dehydration may cause orthostatic hypotension, low blood pressure (manifest by light-headedness, dizziness or fainting upon standing). Protracted and severe dehydration can lead to shock, kidney failure, confusion, acidosis (too much acid in the blood), coma, and even death.
• Moderate or severe bleeding can quickly deplete an individual’s body of blood, leading to low blood pressure or orthostatic hypotension.
• Severe inflammation of organs inside the body such as acute pancreatitis can cause low blood pressure. In acute pancreatitis, fluid leaves the blood to enter the inflamed tissues around the pancreas as well as the abdominal cavity, depleting the volume of blood.
Causes of low blood pressure due to heart disease
• Weakened heart muscle can cause the heart to fail and reduce the amount of blood it pumps. One common cause of weakened heart muscle is the death of a large portion of the heart’s muscle due to a single, large heart attack or repeated smaller heart attacks. Other examples of conditions that can weaken the heart include medications that are toxic to the heart, infections of the muscle of the heart by viruses (myocarditis), and diseases of the heart’s valves such as aortic stenosis.
• Pericarditis is an inflammation of the pericardium (the sac surrounding the heart). Pericarditis can cause fluid to accumulate within the pericardium and around the heart, restricting the ability of the heart to pump blood.
• Pulmonary embolism is a condition in which a blood clot in a vein (a condition called deep vein thrombosis) breaks off and travels to the heart and eventually the lung. A large blood clot can block the flow of blood into the left ventricle from the lungs and severely diminish the ability of the heart to pump blood.
• A slow heart rate (bradycardia) can decrease the amount of blood pumped by the heart resulting in Low blood pressure. The resting heart rate for a healthy adult is between 60 and 100 beats/minute. Bradycardia (resting heart rates slower than 60 beats/minute) does not always cause low blood pressure. But in many patients bradycardia can lead to low blood pressure, light-headedness, dizziness, and even fainting.
One example of bradycardia, sick sinus syndrome, occurs common in the elderly. This syndrome is due to degeneration of the sinus node (SA node), an area in the heart that generates electrical signals that cause the heart to beat regularly. In the sick sinus syndrome, the diseased SA node cannot generate signals fast enough to maintain a normal heart rate. Another condition that causes bradycardia is heart block. Electrical signals from the SA node must travel to the rest of the heart’s muscle to cause the heart to contract and pump blood. Normally these electrical signals are transmitted along special tissues in the heart. Heart block occurs when these specialized tissues are damaged by heart attacks, degeneration that occurs with aging, and medications. Heart block prevents some or all of the electrical signals generated by the SA node from reaching the rest of the heart, and this prevents the heart from contracting as rapidly as it otherwise would.
• An abnormally fast heart rate (tachycardia) also can cause low blood pressure. The most common example of tachycardia causing low blood pressure is atrial fibrillation. Atrial fibrillation is a disorder of the heart characterized by rapid and irregular electrical discharges from the muscle of the heart (instead of the SA node), causing the ventricles to contract irregularly and (usually) rapidly. The rapidly contracting ventricles do not have enough time to fill maximally with blood before the each contraction, and the amount of blood that is pumped decreases, in spite of the faster heart rate.
Medicines that cause low blood pressure
• Medications such as calcium channel blockers, beta blockers, and digoxin (Lanoxin) can slow the rate at which the heart contracts causing Low blood pressure.
• Medications used in treating high blood pressure (such as ACE inhibitors, angiotensin receptor blockers, beta-blockers, calcium channel blockers, and alpha-blockers) can excessively lower blood pressure and result in symptomatic low blood pressure especially among the elderly.
• Diuretics (water pills) such as furosemide (Lasix) can decrease blood volume by causing excessive urination.
• Medications used for treating depression, such as amitriptyline (Elavil), Parkinson’s disease, such as levodopa-carbidopa (Sinemet), erectile dysfunction (impotence), such as sildenafil (Viagra) when used in combination with nitroglycerine, can cause low blood pressure
• Alcohol and narcotics also can cause low blood pressure.
Other conditions that cause low blood pressure
• Vasovagal reaction is a common condition in which a healthy person temporarily develops low blood pressure, slow heart rate, and sometimes fainting. A vasovagal reaction typically is brought on by emotions of fear or pain such as having blood drawn or starting an intravenous infusion.
• Postural (orthostatic) hypotension, as discussed previously, is a sudden drop in blood pressure when an individual stands up from a sitting, squatting, or supine (lying) position. When a person stands up, gravity causes blood to settle in the veins in the legs, hence less blood reaches the heart for pumping, and, as a result, the blood pressure drops.
• Another form of postural hypotension occurs typically in young healthy individuals. After prolonged standing, the individual’s heart rate and blood pressure drops, causing dizziness, nausea and often fainting. In these individuals, the autonomic nervous system wrongly responds to prolonged standing by directing the heart to slow down and the veins to dilate.
• Micturition syncope is a temporary drop in blood pressure and loss of consciousness brought about by urinating. This condition typically occurs in elderly patients and may be due to the release by the autonomic nerves of hormones that lower blood pressure.
• Adrenal insufficiency, for example, due to Addison’s disease, can cause low blood pressure.
• Septicemia is a severe infection in which bacteria (or other infectious organisms such as fungi) enter the blood. The infection typically originates in the lungs (as pneumonia), bladder, or in the abdomen due to diverticulitis or gallstones. The bacteria then enter the blood where they release toxins and cause life-threatening and profound low blood pressure (septic shock), often with damage to several organs.
• Anaphylaxis (anaphylactic shock) is a potentially fatal allergic reaction to medications such as penicillin, intravenous iodine used in some x-ray studies, foods such as peanuts, or bee stings. In addition to a profound drop in blood pressure, individuals may also experience hives, wheezing, and a swollen throat with difficulty breathing.
Symptoms of low blood pressure
- Chest pain
- Weakness
- Lightheadedness
- Heaviness in the eyes
- Tachycardia or rapid heart rate
- Fatigue
- Irregular heart beat
- Fainting
- Decreased urine output
- Nausea
- Weakness
- Depression
- Blurred vision
Some serious symptoms caused due to low blood pressure mainly include:
- Chest tightness
- Chest pain
- Blueness of lips
- Patient may get unconscious
- Unresponsiveness on stimulation
- Palpitation
- Dyspnoea or shortness of breath
- Swelling of the face, tongue, and lips
Diagnosis of low blood pressure
To evaluate the cause of low blood pressure proper, examination of the patient. Examination of pulse, blood pressure, temperature, and respiratory rate should be examined frequently; completely history of the patient including medication, injury or an accident, eating, allergic reaction should be taken with proper attention.
Specific testes mainly include:
- Complete blood count
- ECG
- Urinalysis
- Blood electrolytes measurements
- Chest X-ray
- Holter monitoring
- Cortisol levels to evaluate Addison’s disease
- X-ray abdomen
- CT scan of the chest
- Blood culture
Hypotension, Low Blood Pressure Cases Cured with Homeopathic Medicine
Homoeopathy Can Cure PCOD A Case of PCOD in a Woman of 35 – by Paramjot Saini
A Case of Brain Fog with Hypothyroidism and Hypotension – by Ami Shah





Very informative , comprehensive and helpful.Thank you