Melasma; Mask of pregnancy; Pregnancy mask; hyperpigmentation
– Dr. Rehana Khan
What is Melasma/Chloasma?
A patchy brown or dark brown skin discoloration that usually occurs on face and may result from hormonal changes, as in pregnancy and during the administration of estrogen containing oral contraceptives.
It is generallly found on sun-exposed areas of the face. Melasma often fades over several months after stopping oral contraceptives or hormone replacement therapy(HRT) or after delivering a child. It may return with additional pregnancies or use of these medications. The patches gradually fade over many months. In some people, the discoloration never entirely disappears. However, this condition develops spontaneously in some women who are neither pregnant, taking oral contraceptives, nor HRT medications.
Causes, incidence, and risk factors for Melasma/Chloasma
- Melasma is a very common skin disorder. Though it can affect anyone, young women with brownish skin tones are at greatest risk. Chloasma is especially common in women aged 20-40. It is more common in dark skins than in fair skins.
- Melasma is often associated with the female hormones estrogen and progesterone. It is especially common in pregnant women, women who are taking oral contraceptives (“the pill”), and women taking hormone replacement therapy during menopause.
- Sun exposure is also a strong risk factor for melasma. It is particularly common in tropical climates.
- Melasma develops due to a combination of genetic, hormonal and sun related factors
- Melasma has been referred to as the mask of pregnancy because it often develops during pregnancy. Because of melasma’s relation to pregnancy and oral contraceptives, it is thought that estrogen contributes to its development in predisposed persons.
- Estrogen is not essential to the development of melasma, however, as men may also be affected.
- A factor that does seem to be essential to the development of melasma is sunlight.
- Both ultraviolet A (UVA) and ultraviolet B (UVB) are believed to contribute to the formation of melasma in predisposed persons.
- It may develop in association with menopause, hormonal imbalance and ovarian disorders.
- Melasma may also be triggered by a medication called Dilantin (phenytoin).
- It is thought that female sex hormones causes melanocytes or the pigment-producing cells to produce and deposit excess pigments.
- Chloasma usually affects women but occasionally is seen in young men who use after-shave lotions, scented soaps, and other toiletries.
- Chloasma is more pronounced during the summer months as a result of sun exposure. It usually fades a few months after delivery. Repeated pregnancies, however, can intensify the pigmentation.
- Chloasma also occurs as a side-effect of taking contraceptive pills and injected depot contraceptive preparations. It may also be noticed in apparently healthy, normal, non-pregnant women where it is presumed to be due to some mild and harmless hormonal imbalance.
- Sun exposure, following the use of deodorant soaps, scented toiletries, and various cosmetics can also produce this mottled pigmentation. This is called a phototoxic reaction and is due to ultraviolet radiation being absorbed by the chemical substance on the skin.
- Deficiency of Folic Acid during pregnancy can also lead to development of Melasma.
- Melasma during pregnancy is relatively common. Sometimes it is called the “mask of pregnancy.” The dark patches typically last until the pregnancy ends. Despite the strong connection to hormones, no one knows exactly what causes the skin discoloration.
- Other factors that make it more likely that a person will get melasma include using medications that make you sensitive to the sun (photosensitizing). These can include some cosmetics and medicines used to treat ovarian or thyroid problems. If you are already susceptible to melasma, exposure to the sun increases your risk. For example, women who are pregnant or who take a hormone medication and avoid the sun are less likely to develop melasma than are those who spend a lot of time in the sun.
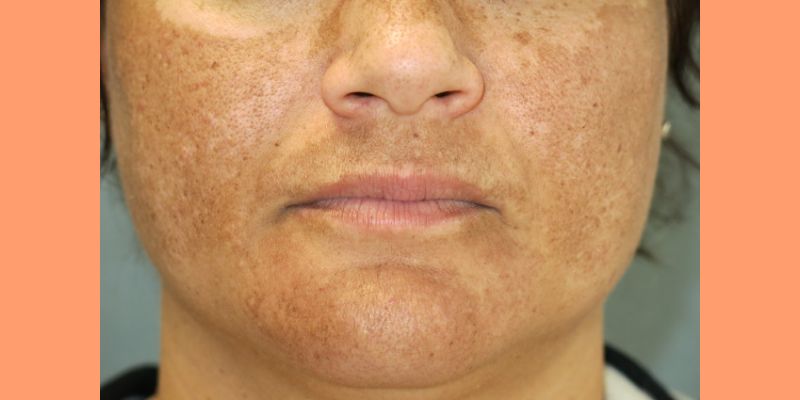
Symptom Pictore of Chloasma / Melasma:
Picture of Chloasms, Melasma
Pigmentation seen on cheeks and nose.
- Tan, dark brown patches
- Irregular in shape
- These patches usually develop on the upper cheek, upper lip and forehead.
- The dark patches often appear on both sides of the face in a nearly identical pattern. The darker-colored patches of skin can be any shade, from tan to deep brown.
- Rarely, these dark patches may appear on other sun-exposed areas of the body.
- The dark patches often appear on both sides of the face in a nearly identical pattern.
- The darker-colored patches of skin can be any shade, from tan to deep brown.
- Rarely, these dark patches may appear on other sun-exposed areas of the body.
- Melasma doesn’t cause any other symptoms besides skin discoloration but may be of great cosmetic concern.
Diagnosis
- Diagnosis is simply done by skin examination.
- Doctor may use a special lamp [Wood’s lamp] that gives off ultraviolet light; it allows the doctor to see patterns and depth of skin discoloration more clearly.
- Medical history will help to determine any factors that may have caused the disorder
Conventional Treatment
- Creams containing tretinoin, kojic acid, and azelaic acid have been shown to improve the appearance of melasma. Occasionally, doctor may recommend chemical peels or topical steroid creams.
- In severe cases, laser treatments can be used to remove the dark pigment.
HOMEOPATHY TREATMENT & HOMEOPATHIC REMEDIES
Homeopathy treats the person as a whole. It means that homeopathic treatment focuses on the patient as a person, as well as his pathological condition. The homeopathic medicines are selected after a full individualizing examination and case-analysis, which includes the medical history of the patient, physical and mental constitution etc. A miasmatic tendency (predisposition/suceptability) is also often taken into account for the treatment of chronic conditions. The medicines given below indicate the therapeutic affinity but this is not a complete and definite guide to the treatment of this condition. None of these medicines should be taken without professional advice.
Reportorial rubrics:
[Kent] skin, discoloration, brown, liver spot
[Kent] skin, discoloration, brown, chloasma
[Murphy] skin, chloasma
[Boericke] skin, chloasma, liver spots, moth patches
[Boenninghausen’s] Skin, Spots, Liver (brown, liver-colored, chloasma)
Commonly indicated Homeopathy medicines
- Sulphur,
- Lycopodium clavatum,
- Sepia offincinalis,
- Thuja occidentalis,
- Argenticum nitricum,
- Cadmium sulphuratum,
- Copaiva offincinalis,
- Guarana,
- Kali bromatum
- Sarsaprilla
- Phosphorus
- Petroleum
- Rhus toxicodendron
- Silicea
- Graphitis
- Nitric acid
- Caulophyllum,
- Thalictroides,
- Plumbum metallicum,
- Curare.
Homeopathic Remedies:
Sulphur
- Skin affection after local medication.
- Old looking. Spotted face.
- Skin dry, rough, wrinkled, scaly; Itching, violently at night.
- Unbreakable itching, especially from warmth.
- Dirty, filthy people, prone to skin affection.
- Very unhealthy skin, even small injuries do not heal quickly.
- Patient looks dirty and avoid bathing.
- Violent itching in any skin complaint.
- Strong desire for sweet.
- Burning in skin.
Lycopodium Clavatum
- Grayish-yellow discoloration of the face with blue circles around the eyes.
- Brown spot on face and nose.
- Skin eruption specially on right side of the body
- Skin eruption associated with liver and gastric complaints.
- All skin complaints worse from warm application.
- Yellow and offensive sweat.
- Premature graying hairs
- Dryness associated with every skin complaint.
- Craves everything warm.
- Patient is very anxious,
Sepia Offincinalis
- Chloasma; yellow spots [moth spots] the on the face, and a yellow saddle across the upper part of cheeks and nose.
- Suited to patient with having dark hair, rigid fibre.
- Ailments during pregnancy.
- Acne specially due to hormonal disturbance in female.
- Acne associated with menstrual disturbances.
- Mentally patient is very anxious about family or may be indifferent to family.
Thuja Occidentalis
- Dry skin with brown spot.
- Skin looks dirty.
- Face, pale, waxy, shiny; dark under eyes; spiderlets on.
- Offensive perspiration.
- Patient has craving for raw onion.
- Mentally patient has fixed ideas.
- May have history or sexual infection.
Argenticum Nitricum
- Face looks sunken, old, pale and bluish.
- Brown liver spot; irregular blotches.
- Skin is brown, tense and hard.
- A prematurely aged look.
- Very anxious patient, anticipate everything.
- Patient has strong desire or aversion for sweet
- Fear of high places.
Sarsaprilla
- Melasma, skin discoloration specially in summer weather.
- Old, shrivelled skin.
- Wrinkled skin.
- Eruption all over the body, usually one sided and especially right side. Right side of nose, right wrist, right ankle etc.
Cadmium sulphuratum
- Chloasma, yellowish stains on nose and cheeks;
- Worse from exposure to sun and wind.
Copaiva Offincinalis
Brown spot; circumscribed, lenticular patches with itching. Mottled appearance.
Guarana
Chloasma on temples and arms. intellectual excitement; uncontrollable sleepiness.
Caulophyllum Thalictroides
Discoloration of skin in women with menstrual and uterine disorders.
Plumbum metallicum
Yellow, corpse like dark brown liver spots; cheeks sunken. Skin of face is greasy, shiny. Face pale cachetic.
Curare
Red face. Dirty looking skin. Melasma.
Prevention of Chloasma, Melasma.
- Avoiding the sun and using sunscreen are key to preventing melasma.
- Avoid irritating the facial skin- No strong soaps or abrasive cleaners – use only a mild soap or cleanser for washing.
- Increase intake of foods high in folic acid, dark green leafy vegetables, wheat germ, asparagus, broccoli, potatoes, whole grains, fruits and vegetables.



Very good information about Melasma.. I will try Lycopudiam..Thanks
Mem, meri age 37 year hai meri skin oily hai ,mera complexion fair tha, face gora chamkdar aur sundar tha, parantu 8-10 month se achanak meri skin dark honi shuru ho gayi aur in dino to mera face bahut adhik dark brown looking ho gaya hai aur chehre per sikudan bhi aati ja rahi hai, jis se meri age ab 50-55 ki tarah lagne lagi, mai kaun si cream aur dawaye use karu jis se mere chehre ki khoyi raunak vapas aa jaye ? Kripya meri taklif dur kar dijiye, Mai aapka jivan bhar ehsanmand rahuga
Very scientific and easy to understand information.
Thanks, to bring in at one article
I have a client who has been diagnosed with Melanoma cancer. Are there any peer reviewed cases where this condition was cured through homeopathy alone?
Which medicine to cure sir